In 2019, harmed patients mounted a class-action lawsuit against Clarence Nabers, DDS. Patients allege Nabers negligently infected them with Hepatitis B (HBV) when he didn’t sterilize needles properly.
Nabers also exposed patients to other bloodborne pathogens with his risky behavior. The class claims Nabers re-used single-use instruments and did not follow sanitation mandates.
The Tennessee Board of Dentistry suspended Nabers’ license to practice for two years. Now, the non-compliant dentist might face a harsh penalty: a settlement for $50 million.
Nabers is facing the consequences of his reckless choices. Tragically, so are his patients. Bloodborne pathogens like HBV cause lifelong, sometimes lethal problems.
15-25% of HBV patients develop severe liver problems. 3000 people in the United States die of HBV every year. The good news is, bloodborne pathogen transmission is preventable.
Dentists can prevent transmission with bloodborne pathogens training. Bloodborne pathogens training enables dental offices to meet the BBP Standard and to save patients’ lives.
OSHA Sets Bloodborne Pathogens Standard
The Occupational Health and Safety Administration (OSHA) set the Bloodborne Pathogens Standard (BBP) in 1991. Since then, they’ve continually updated the set of regulations.
The BBP Standard mandates practices that prevent bloodborne pathogen transmission in high-risk settings. In 2000, OSHA amended the Standard with the Needlestick Safety and Prevention Act.
This update ensures medical staff use needles in the safest way possible, to prevent pathogen transmission. OSHA enforces the BBP Standard with fines and penalties.
Patients may file a lawsuit against any practice that violates the BBP Standard. Twenty-eight states enforce laws that regulate needle use and other risky practices.
All high-risk workplaces must meet the BBP Standard. This includes any workplace where an employee “reasonably expects” to encounter blood. Meeting the BBP Standard is mandatory for:
- hospitals
- nursing homes
- tattoo studios
- medical practices
- dental offices
- other healthcare practices
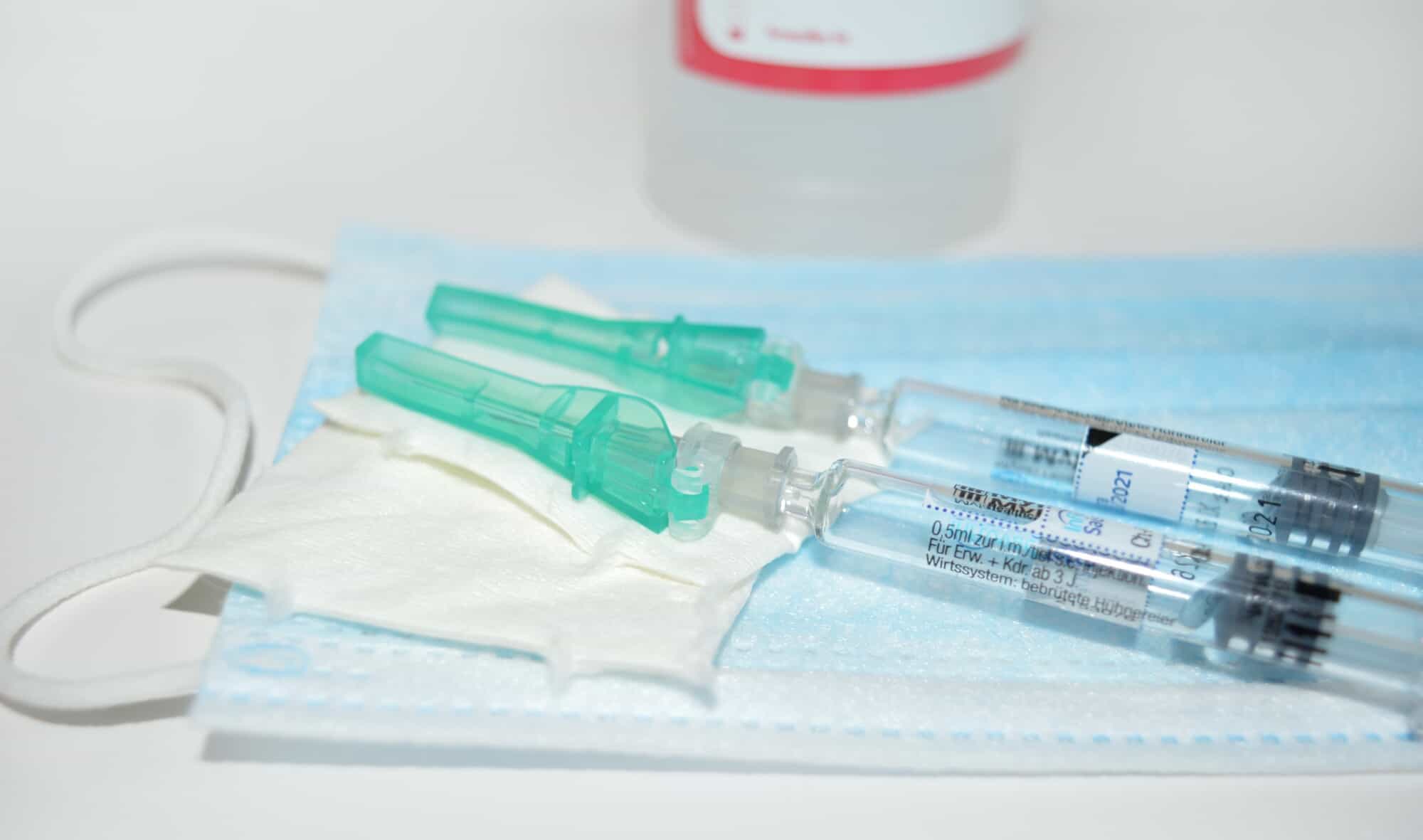
Accidental needlesticks and unsanitary needle practices can transmit bloodborne pathogens. As seen in the example of Clarence Nabers, DDS, Hepatitis B can pass from one person to another via a medical needle.
Fortunately, any practice can implement safer needle practices. You can improve your office’s needle safety in dental practices with some tips and strategies.
How to Reduce Accidental Needlesticks
OSHA publishes recommendations on how to reduce accidental needlesticks on its official website. This is a brief rundown of the administration’s recommendations that meet the BBP Standard.
There are five strategies to reduce the risk of transmission. Dental offices can implement all of them.
1. Use Universal Precautions and PPE
The CDC standardized Universal Precautions in the 1980s. These precautions aimed to prevent the spread of HIV/AIDS at the height of the epidemic.
OSHA adopted the Universal Precautions into its Bloodborne Pathogens Standard in 1991. Universal Precautions require medical practitioners to consider all blood and other potentially infectious materials (OPIM) to be infectious.
One set of precautions requires anyone who might contact blood or OPIM to wear Personal Protective Equipment (PPE). PPE includes pathogen-resistant gowns, BBP Standard masks, gloves, and protective eyewear.
Protective clothing prevents fluid-based transmission. It creates a barrier between any fluid and the practitioner’s skin and mucous membranes.
2. Implement Engineering Controls
In general terms, engineering controls are practices and design choices in a workplace that reduce the risk of bloodborne pathogen transmission. Some practices are widespread, like hand-washing mandates.
Others are unique to specific workplaces. There are engineering controls that prevent pathogen transmission via laundry, for example. In this case, we will look at engineering controls specific to needlestick risks.
2a. Use Safer Needles
Invest in safer needles for your office. To evaluate needle safety, make notes of any needlesticks in your office. Then, note variables that factored into the accident.
Select needles and devices that eliminate those variables. To further your research, look at conclusions drawn by the Exposure Prevention Information Network (EPIN). This network compares needle designs and outcomes to determine best practices.
Engineers develop new medical technology every day, so it’s good to periodically research and update your inventory. Here are some of the options recommended by OSHA, the CDC, and EPIN.
- Self-sheathing needles
- Safer medical devices
- Retractable technology
- Needleless connector system for IVs
- Hinged or winged safety needles
You can learn more about each safety option on OSHA’s official site. OSHA also provides animated demo videos, so you can see each feature in action.
2b. Use Safer Sharps Containment
Make it easy to dispose of used sharps safely, instantly. Engineer the interior space with many, easily accessible sharps disposal containers. The best interior design will keep sharps disposal containers within arms reach at all times.
Alongside this, implement a standard practice of immediately disposing of used sharps. Or enforce the practice of immediately containing sharps after use if they are meant to be reused after sterilization.
Poor sharps containment is the leading cause of accidental needlesticks in medical practices. In surveys, 73% of medical staff felt their practice did not have enough sharps containers, and the ones they had were poorly placed.
Best Sharps Containers
Sharps containers must be safe and usable. OSHA, the CDC, and the FDA mandate the following engineering controls for sharps containers. Sharps containers must have the following qualities:
- puncture-resistant plastic or metal material
- leak-proof sides and bottom
- tight-fitting lid
- vertical placement (lid on top)
- stable upright design
- accessible
- labeled according to OSHA guidelines
- red or orange (vibrant/fluorescent)
- marked with biohazard symbol
Please read all FDA and OSHA guidelines on sharps container requirements. Labeling mandates vary, so be sure to apply the correct notation to your containers.
Best Sharps Containment Practices
The best practices ensure that the sharps container is easy to access as soon as a sharp is used. This means the container must be present, and it must not be full.
Thus, to optimize sharps containment, you need to implement routine container disposal. When sharps have filled the container to the three-quarter line, dispose of it.
To dispose of a sharps container safely, follow medical waste disposal guidelines. Sharps container vendors and local regulations determine and distribute these guidelines.
Finally, consider mobile or portable sharps containers. An employee may set up a portable sharps container beside them as they use a needle. Then, the employee can instantly dispose of the needle after use, in one movement.
After the employee disposes of the needle, they can easily move the portable sharps container out of the way.
3. Needle Training
Needle training lets employees practice the optimal ways to handle and dispose of sharps. Staff might handle sharps to do vaccinations, draw blood, or connect a needle to an IV.
While there are basic similarities in those circumstances, there are also differences that can lead to accidents. As such, it’s good to implement routine guided needle training. Employees can get feedback on their needle-handling techniques from professionals.
4. Regularly Update Exposure Control Plan
An exposure control plan is a written document. It notes specific standards and practices that an office mandates to prevent bloodborne pathogen transmission.
Exposure control plans mitigate the risk of pathogen exposure for any employee or patient. They also note how to isolate a biohazard (blood or OPIM) in the event of an accident.
Finally, exposure control plans note what to do in the event of an exposure. The plan outlines:
- sanitation steps
- documentation
- how to inform OSHA
- how to inform any affected patients or staff
- how and when to follow up with affected individuals, post-exposure
As threats emerge, an exposure control plan must adapt. Likewise, new technological developments and scientific insights can benefit your office. This is why OSHA requires offices to check and revise their exposure control plans at least once per year.
OSHA mandates yearly Bloodborne Pathogens Training. Many offices choose to update their exposure control plans during those sessions.
5. Keep Records
OSHA outlines recordkeeping regulations in this document. Medical practices must record all sharps injuries. Records must include:
- the date
- the type of device that caused the injury
- the device’s brand
- the specific workplace area where the injury happened
- a brief explanation of how the incident happened
Keeping track of sharps injuries empowers you to recognize patterns. So, you can intervene to prevent injuries more effectively.
OSHA also requires offices to keep other records and communicate actively to reduce risks. Practices must record declarations from any employee who is not vaccinated for HBV. They must also meet regulations when they communicate about hazards.
Beyond Needlestick Prevention
These guidelines can help a dental office meet BBP standards. But they aren’t all-encompassing. OSHA updates the BBP Standard as new threats emerge, and as engineers develop new technology.
Moreover, the BBP Standard aims to prevent pathogen transmission in all its forms, not only needle-based transmission. As such, OSHA requires all relevant employees to attend Bloodborne Pathogens Training once per year.
How to Reduce Bloodborne Pathogens
The best way to learn how to reduce bloodborne pathogens is to take the bloodborne pathogens training guide. Bloodborne pathogens training is a mandatory, annual continuing education seminar.
These classes keep medical practitioners up-to-date on new amendments to OSHA’s BBP Standard. Trainers also offer examples and practical strategies to implement. This way, any organization can minimize transmission risks.
Dental Office Bloodborne Pathogens Training
Dental offices face unique transmission risks. Dentists work directly inside a patient’s largest mucous membrane. Simultaneously, dentists run on a tight schedule.
The typical dentist sees ten to fifteen patients in an eight-hour day. Unpredictable variables make exams run long. This leaves staff with very little time to perform pathogen prevention tasks.
Fortunately, there are Bloodborne Pathogens Training seminars that address dentist’s unique circumstances. Complying with both OSHA and HIPAA in this context requires strategizing.
Dental office staff can learn how to prevent bloodborne disease, even under tight deadlines.